Trichotillomania And N-acetylcysteine
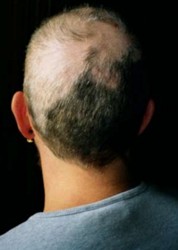
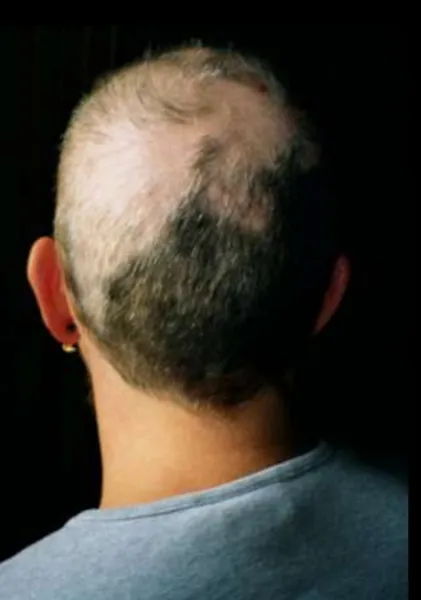
Trichotillomania, which is classified as an impulse control disorder by DSM-IV, is the compulsive urge to pull out one's own hair leading to noticeable hair loss, distress, and social or functional impairment. It is often chronic and difficult to treat.
Trichotillomania may be present in infants, but the peak age of onset is 9 to 13. It may be triggered by depression or stress.
Due to social implications the disorder is often unreported and it is difficult to accurately predict its prevalence; the lifetime prevalence is estimated to be between 0.6% (overall) and may be as high as 1.5% (in males) to 3.4% (in females).
The name, coined by French dermatologist François Henri Hallopeau, derives from the Greek: trich- (hair), till(en) (to pull), and mania ("an abnormal love for a specific object, place, or action").
Our brains can give rise to all manner of odd psychiatric problems, but one of the strangest is trichotillomania which is better known as hair-pulling.
The uncontrollable desire to yank out one's hair may seem unusual, but the disorder is actually not so uncommon. Estimates of the number of Americans with trichotillomania range as high as eight million, although Dr. Swedo, a researcher at the National Institute of Mental Health said two million to four million is probably more accurate. Virtually all are women.
Exact numbers of trichotillomania are hard to come by since people with the condition often hide it. Sometimes they don't even appear in public because they're not able to camouflage their various bald spots.
As a psychiatric disorder, hair-pulling is among the earliest recorded chronic problems. Humans seem wired to attack their hair under traumatic conditions.
The reason is not completely clear but experts believe it's possibly because forcibly extracting hair is painful. When humans feel pain from pulling out their hair it may actually divert attention from other stresses to the more immediate matter of how to solve a pressing problem.
For chronic hair pullers, that diversion turns into addictive psychological relief. Some people with trichotillomania pull out hairs not only from their heads but also from their pubic areas and armpits; as many as 20% eat their hair; a small minority pull other people's hairs. "Many say it's not painful but more of a sense of just a tug, one that provides a calming feeling," says Grant.
"Some of these people are not even aware they are pulling their hair. Their spouses will say, 'Stop that,' and they are not even aware they have a clump of hair on their lap."
Medication
There is no approved treatment. Currently, most patients with trichotillomania are treated with psychotherapy or antidepressants, including selective serotonin-reuptake inhibitors (SSRIs), like Prozac.
Traditional treatment is often with clomipramine (Anafranil), a tricyclic antidepressant, has been shown in a small double-blind study to significantly improve symptoms, but results of other studies on clomipramine for treating trichotillomania have been inconsistent.
Fluoxetine (Prozac) and other selective serotonin reuptake inhibitors (SSRIs) have limited usefulness in treating trichotillomania, and can often have significant side effects.
Behavioral therapy has proven more effective when compared to fluoxetine or control groups.
Dual treatment (behavioral therapy and medication) may provide an advantage in some cases, but robust evidence from high-quality studies is lacking. Acetylcysteine treatment stemmed from an understanding of glutamate's role in regulation of impulse control.
SSRIs May Not Be Effective For Hair Pulling Condition
But in recent years, four studies that looked at SSRIs in the treatment of trichotillomania showed they are not effective in relieving the condition. (Indeed, there is an emerging debate about the limitations of SSRIs, which received enormous media exposure in the '90s and have become the go-to drug to treat not only depression but, with varying success, anxiety, nicotine addiction, body-image problems, bipolar disorder, psychosis and a host of other mental disorders.)
While there's been less research on drugs that manipulate glutamate — perhaps because it can be modulated fairly easily with nonprescription amino acids like N-acetylcysteine — the new study suggests the neurotransmitter may play a key role not only in the rare condition of hair-pulling but also in other obsessive-compulsive problems.
Many medications, depending on individuality, may increase hair pulling.
Does N-acetylcysteine Help?
If the findings bear out, they may herald a potential new treatment for an age-old condition.
A research paper published in the prestigious Archives of General Psychiatry offers a simple new hope for trichotillomania sufferers.
In a small trial of 50 hair pullers, more than half of those who took an over-the-counter antioxidant called N-acetylcysteine, which is available in pill form at mainstream stores, had improvement of symptoms after 12 weeks, compared with 16% of those taking a placebo.
Experts theorize that trichotillomania may be a kind of grooming irregularity that falls into the obsessive-compulsive family of disorders. "Some parrots pull out all their feathers," he says. "Some mice pull out all their fur."
Reduction in Glutamate
That may explain why the antioxidant N-acetylcysteine can help prevent it. The compound is thought to work by reducing the synaptic release of a neurotransmitter called glutamate.
Glutamate is the communication chemical that "tells the brain, 'Do it! Do it! Do it! Do it!' And the rest of the brain can be overwhelmed by this drive state."
Reduce glutamate and you may reduce the drive state. Previous studies have suggested the supplement may also reduce urges to use cocaine and to gamble.
In the 12-week study, those compulsive hair pullers who were randomly assigned to receive 1,200 to 2,400 milligrams of N-acetylcysteine a day experienced a 40% reduction in scores on a test designed to measure trichotillomania.
Is N-acetylcysteine the answer? Of course the jury is still out, but some experts in the trichotillomania field are trying alternative methods of treating this puzzling compulsive disorder. Those alternative treatments might include nutritional counseling combined with N-acetylcysteine and other behavioral modification sessions.
The good news about the success with N-acetylcysteine is that it opens new possibilities for finding successful treatments for the hair pulling compulsion.Social Media Network Information
Please follow us on Twitter at: https://Twitter.com/HairBoutique. I look forward to meeting new people from all walks of Twitter and learning from their Tweets.